|
Investing Wisely in Health: Considerations for the Caribbean

Karl Theodore and Anton Cumberbatch
HEU, Centre for Health Economics, University of the West Indies, St Augustine, Trinidad
E-mail: Karl.Theodore@sta.uwi.edu
Abstract
The paper advocates directing investment in the health sector to two major areas: primary health care/public health care and in health system efficiency. It discusses this investment in the context of shrinking economic resources and the heavy presence of non-communicable diseases (NCDs). The authors argue that targeted investments in primary and public health, aimed at preventing and reducing the prevalence of NCDs can lead to Caribbean governments recouping significant returns that can amount to billions of dollars. Further, effective management of an efficiently run health information system can result in cuts in wastage of approximately US$2 billion.
Keywords: Investing in health, NCDs, CARICOM
Introduction
The English-speaking Caribbean region comprises a number of small countries with populations ranging between five thousand in Montserrat and 2.8 million in Jamaica (www.worldometers.info). The combined national income of the region has been estimated in 2015 at US$70 billion, with the range of per capita income between US$3,993 (Guyana) and US$42,300 (British Virgin Islands). The health expenditure in the region averages just about 6% of GDP, with the range of per capita health expenditure between US$250 (Guyana) and US$1,621 (Bahamas). The region is not one of poor countries but nearly every country faces serious fiscal deficits and significant levels of debt.
In a context of shrinking economic resources, the mandate for governments to spend and invest wisely across the spectrum of services offered to their populations is paramount. In the English-speaking Caribbean, this requirement is particularly important given the vulnerabilities of many of these economies, which are largely dependent a single export product. In 1993, the World Development Report titled Investing in Health made the case for more targeted investments in health since it was a critical factor the development of nations (World Bank, 1993). Two years prior, Over (1991) highlighted key linkages between the health sector and the rest of the economy and maintained that the health of the population, through direct and indirect means, impacted a country’s capacity to produce and renew wealth and ultimately, its level of welfare or development.
Apart from the economic bonuses of good health, a more critical and basic goal is the improved quality of life of the citizens of these nations. In this paper, we argue that countries in the region should focus their investment in health in two main areas. The first area we advocate is investment in Primary Health Care and Public Health facilities and programmes for keeping the population healthy, as opposed to spending mainly on Secondary/Tertiary care institutions. Secondly, investing in keeping the health system efficient is essential for maintaining the required functions of the system. In looking at both these areas we ask the following three questions to expand the discussion:
- Why the investment bias?
- Who should make the investment?
- What are the measurable expected returns?
We now discuss both recommendations, each in the context of the three questions.
Investing in Primary Care and Public Health
- The Bias of Investing in Primary Care and Public Health
The single most important reason for proposing a new bias in health investment is the growing burden of non-communicable diseases in all our countries. The fact is that these are diseases where prevention, early diagnosis and proper management have major implications for both health status and cost of health care. Further, new hospitals will not constitute an adequate response to the problem of non-communicable diseases (NCDs) in our countries. According to the Pan American Health Organization (PAHO), “In the Caribbean, non-communicable diseases (NCDs) and their risk factors were responsible for 78% of all deaths in 2010” (PAHO, 2015). The bias for health investments in the future needs to be in facilities, personnel and equipment that elevate the quality of services aimed at controlling and managing the NCDs—precisely the area covered by primary care and public health.
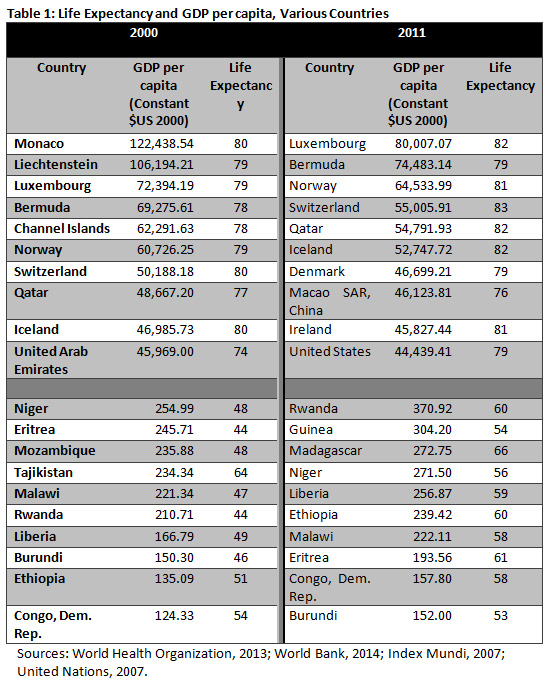
We have known for quite some time that the good health of the population was a standard objective of development. As living standards improve, we expect a similar change in health status. What has been more recently determined is that countries will not attain the level of development they are aiming for except they ensure that the health status of the population is duly enhanced. A look at global country data also seems to indicate that there is a positive relationship between improved health status, proxied here by life expectancy, and higher levels of development, proxied by GDP per capita (Table 1).
Bloom et al. (2004) using their full income model, argue that declines in mortality (in other words, improvements in health) lead to an appreciation of human capital, which in turn leads to an enhancement of the quality of life of the population. Further, they maintain that low mortality rates provide incentives for persons to save, since the prospect of a longer life leads to financial planning for the future. So, while we always knew that development was good for health, we now know that health is good for development. This, in a nutshell, is the reason why investing in the good health of the population makes sense.
- Who Should Invest in Maintaining Population Health?
It is important to address the question of responsibility for population health. Who should be required to make the necessary investments? While government obviously must bear significant responsibility here, if the investment target is population health it does not make sense to leave this to the government alone. The truth is that there are other major stakeholders who benefit greatly from good population health.
There is a warranted role here for the business sector. This sector is a major beneficiary of development. With labour and capital as the main factors of production and, by implication, the main pillars of generating profits, there is no question that it is a healthy population that will provide a healthy labour force and reduced expenditures on treatment, which impact negatively on capital accumulation. Diagram 1 illustrates.
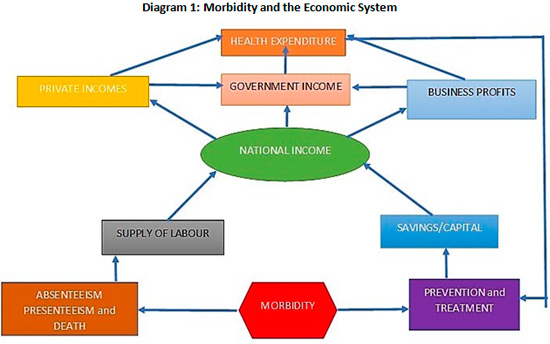
The diagram shows that while morbidity impacts on the supply of labour through absenteeism, presenteeism and death, it impacts on capital (accumulated savings) by the expenditures incurred for prevention and treatment of illness. These impacts on the factors of production carry through to the national income, which is the source of all other incomes—private, government and business. These incomes, in turn, affect the level of health expenditure, which in turn, will determine how much prevention and treatment is possible.
Supporting the role of the business sector should be the social security organizations (SSOs). Since the labour force of the country is the contribution base of the SSOs, they will have an interest in protecting the health of their contribution base, and an equivalent interest in minimizing the level of health claims by contributors. Given the lifelong link that SSOs have with contributors, and the information base which is at their disposal, it would be convenient for the SSOs to monitor and make recommendations in respect of the health of their contributors at the stages when specific attention to health matters is required. One area where it would therefore make sense for the SSOs to take the lead is in the setting up of national healthy aging programmes.
As it pertains to healthy aging, we know that where NCDs are concerned, the three key target groups are:
- those not affected by disease,
- those with early or mild onset of disease, and
- those with serious complications of disease, including comorbidities.
This makes it necessary for countries to adopt a range of programmes aimed at these various groups, to promote healthy aging of the population. If countries are successful in the healthy aging approach by ensuring that the working population pay attention to healthy lifestyles and risk reduction behavior, the benefit will be an extended life span. The healthy older (pensionable) citizens can remain being productive and involved in their own revenue generating activities, giving a new twist to the notion of retirement.
Healthy aging programmes will help tremendously with positive mental and physical health and will ensure that worker experience will be a perceptible contributor to the development of all our countries, allowing the elderly to remain relevant and useful to the society. It is important to note that with the involvement of the SSOs, and with them taking leadership for healthy aging, this will be an investment in health which would yield measurable returns.
- Measurable Expected Returns of Investing in Primary/Public Health Care
There are several ways of looking at the returns to keeping the population healthy. Available data tell us that the NCDs are imposing a cost of at least 4% of GDP in lower middle income countries (LMICs) where studies have been done (Chao, 2013). If this percentage holds for the region, we will be facing an NCDs cost of over US$2.7 billion. However, if our investments save us even a fraction of this the returns will be significant. Over time, these returns will account for many billions of dollars which will be compounded by measures taken to make the health systems function more efficiently. It is important to understand these returns. It can be argued that investment in health yields two separate but related streams of returns:
- one stream contributes to the state of health enjoyed as a result of the investment; and
- the second stream contributes to the productivity impact on the national income.
There is more than a prima facie case for skewing health investment in the directions suggested. There is no argument that early preventative intervention via the Primary Health Care system brings the highest returns in terms of avoided mortality and reduced to no morbidity impact. This will translate into positive impacts on labour productivity and output. As shown in the Diagram 2 the No Intervention option brings with it the highest risk of mortality and morbidity effects and the highest likelihood of entry into the secondary health care system with reduced productivity levels being the likely outcome. This option brings significant costs to the health system and huge losses in terms of productivity and output reductions. Secondary intervention is assumed to be mainly neutral to productivity.
We are now in a position to understand how the returns to health investment arise. As we have seen earlier, the impact of morbidity on the national income works through the labour force and the accumulation of capital (savings). We also know that there are three channels through which primary care reduces hospital admissions: preventive and promotive activities, secondary preventive activities, early detection activities.
Diagram 2 suggests that a good working hypothesis is that the investment returns are highest for primary care and public health/health promotion. Our expectation is that vertical targets are third and that last on the list would be secondary/tertiary care. On the one hand, the reason for this ranking is allied to the case that can be made linking primary care and public health to labour productivity and capital accumulation. On the other hand, the demographic profile of hospital admissions suggests that many of the persons admitted are already out of the labour force, making the output of hospitals neutral to productivity.
Investing in Keeping the Health System Efficient
- The Case for Investing in an Efficiently Run Health System
The main purpose of attaining and sustaining efficiency in the health system is to guarantee the capacity of the health system to properly deliver needed services to the population. If the cost of the system spirals out of a feasible range the impact on the quality of life of the population would be near catastrophic. In a situation where the cost of health care in most countries is already increasing at an exponential rate, and certainly at a rate higher than the rate of growth of the countries, the prospect of having to deal with an epidemic of NCDs is certainly one that has to be addressed. Without health system efficiency, a future with adequate health coverage will fade into impossibility.
There are two main investment requirements if health system efficiency is the target. The first is the adoption and implementation of a modern health information system (HIS) to keep track of cost generation in every aspect of the health system. According to the WHO, “sound and reliable information is the foundation of decision-making across all health system building blocks, and is essential for health system policy development and implementation, governance and regulation, health research, human resources development, health education and training, service delivery and financing” (WHO 2008, p.2).
The second requirement is the installation of a high-calibre management cadre to ensure that value for money is derived from the human resource and procurement functions. Stansfield (2005) indicates that in the health sector, the way in which data generated from an HIS is managed “will determine the system’s effectiveness in detecting health problems, defining priorities, identifying innovative solutions and allocating resources to improve health outcomes.” HIS management is therefore a basic yet critical function if the gains we desire from an efficiently run health system are to be achieved.
- The Returns from an Efficient Health System
Returns from health system efficiency will be manifest in two ways: the impact of cost control on the trend in overall health expenditure and the impact on the quality of service provision both in respect of the time required and calibre of the outcomes. The public goods nature of these returns suggests that the investment in system efficiency should be spearheaded by the public sector with support from the private sector.
The WHO (2010, p. 79) has indicated that the waste in health spending is of the order of 20% to 40%. For the Caribbean, with health spending just under US$5 billion, and using the upper boundary, countries could be losing close to US$2 billion. This is what is at stake.
Conclusion
In the Caribbean context, the important role health plays in income generation and overall development in the region was captured in the Nassau Declaration on Health 2001 by CARICOM Ministers of Health in The Bahamas, where they indicated that they were “cognizant of the critical role of health in the economic development of our people and overawed by the prospect that our current health problems, especially HIV/AIDS, may impede such development through the devastation of our human capital...” (http://www.caricom.org). This view also extends to the impact of NCDs on the populations of these countries as is evidenced by the meeting of Caribbean Health Ministers and the Caribbean Public Health Agency (CARPHA), at the 69th World Health Assembly in 2016, at which they discussed a way forward to counteract the prevalence of NCDs, in particular the epidemic of heart disease, strokes, diabetes and cancer (http://carpha.org).
The basic message is that if the reality of the NCD epidemic in the Caribbean is to be addressed in an effective manner, a major policy change in respect of health investment is called for, with primary care and public health taking centre stage and with a significant commitment to the establishment of health information systems.
References
Bloom D, D Canning and DT Jamison (2004). Health, Wealth and Welfare. Finance and Development, 41(1):10-15.
Chao, Shiyan (2013). Economic Impact of Noncommunicable Disease in the Caribbean. Presentation at the Caribbean Health Financing Conference, Jamaica (www.nhf.org.jm).
Index Mundi (2007). Liechtenstein Life Expectancy at Birth [website] (www.indexmundi.com).
Over, Mead (1991). Economics for Health Sector Analysis: Concepts and Cases. EDI Technical Materials. Washington D.C., World Bank.
PAHO (2015). NCDs in the Caribbean. PAHO/WHO.
Stansfield, S (2005). Structuring Information and Incentives to Improve Health. Bulletin of the World Health Organization, 83(8):562.
United Nations (2007). World Population Prospects: The 2006 Revision. Highlights. Department of Economic and Social Affairs Population Division. New York, United Nations (www.un.org).
World Bank (1993). World Development Report: Investing in Health. New York, Oxford University Press.
World Bank (2016). World Development Indicators database (data.worldbank.org).
World Health Organization (2008). Toolkit on Monitoring Health Systems Strengthening: Health Information Systems. Switzerland, WHO (www.who.int).
World Health Organization (2010). The World Health Report: Health Systems Financing: The Path to Universal Coverage. Switzerland, WHO.
World Health Organization (2013). Global Health Observatory Data Repository. Switzerland, WHO (apps.who.int).
World Health Organization (2016). Global Health Expenditure database. Switzerland, WHO (see apps.who.int).
Deja tu opinión:
|